STOCKHOLM, Sweden: Ten years ago, Sweden did away with the recommendation of administering antibiotics prophylactically for patients deemed at risk of contracting infective endocarditis (IE) caused by oral viridans group streptococci (VGS) during certain dental procedures. According to the results of a recently published longitudinal study, the number of cases of such IE in these patients did not increase despite the near cessation of antibiotic prophylaxis. The researchers suggested that these results provide further evidence that the use of antibiotics for prevention of IE could be discontinued in dentistry.
The purpose of the study conducted by Swedish researchers mainly from Karolinska Institutet in Stockholm was to determine whether there was an increased incidence of VGS IE in high-risk patients after Sweden implemented antibiotic prophylaxis reduction in October 2012. Patients considered at risk of IE are those who have received a prosthetic heart valve, who have had endocarditis previously or who have congenital heart disease. Over the course of a ten-year period, over 70,000 patients, aged 17 and older, who were deemed high risk for IE were evaluated. Nearly 400,000 patients who were considered low risk were also evaluated over the same period. To avoid survivorship bias, the high-risk patients were stratified into a prevalent cohort if the date of first diagnosis of a risk factor for IE was before 2008 and to the incident cohort if they became high risk during the study period.
Co-author of the study Niko Vähäsarja, who is a PhD student and dentist at Karolinska Institutet, said that the research found no signficant indications of increased morbidity in patients at high risk of IE since Sweden moved to reduce antibiotic use, a move meant to reduce antibiotic resistance and borne of a lack of evidence of its necessity. In the prevalent cohort (36,158 patients; 57% male), 395 (1.1%) had developed IE after ten years. In the incident cohort (36,363 patients; 61% male), 516 (1.4%) had developed IE after two years.
“Our study therefore supports the change in recommendation. This is an internationally debated issue and Sweden and the UK are the only countries in Europe to restrict antibiotic use like this,” he concluded.
Vähäsarja said that the next logical step in this course of research would be to use the data the researchers had collected from the various Swedish public health authorities to look deeper into what dental procedures those in the high-risk group underwent during the period covered by the study. Vähäsarja indicated that such data could help aid other countries’ medical authorities as they strive to make decisions regarding antibiotic use as well.
According to a recent joint report by the World Health Organization and the European Centre for Disease Prevention and Control, the number of deaths in the EU/European Economic Area resulting from antimicrobial resistance equals that stemming from HIV/Aids, tuberculosis and influenza combined, a total of about 33,000 individuals. Worldwide, IE cases have skyrocketed in the past 30 years, according to recent research published in Frontiers in Medicine. Documented cases of IE reached 1,090,530 in 2019, compared with 478,000 in 1990. Resulting deaths from IE increased to 66,320 from 28,750 for the same years.
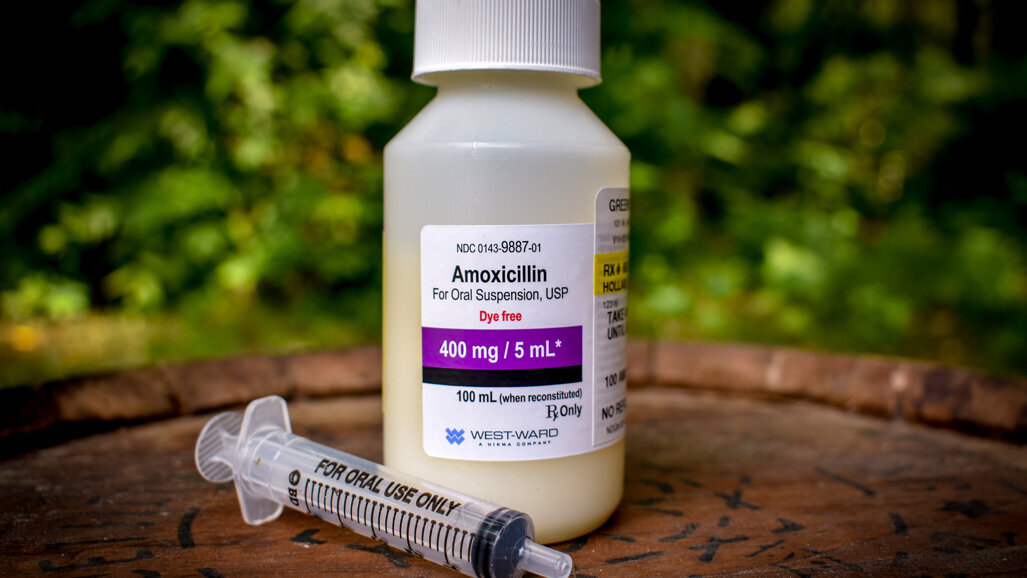
Amoxicillin prescriptions for dental purposes have dropped by 40% in Sweden since October 2012.
The study, titled “Infective endocarditis among high-risk individuals—before and after the cessation of antibiotic prophylaxis in dentistry: A national cohort study”, was published online on 4 February 2022 in Clinical Infectious Diseases ahead of inclusion in an issue.
Tags:
LONDON, UK: According to a new study, dentists in England wrote 25% more prescriptions for antibiotics between April and July 2020 than they did during the ...
According to Dr Wendy Thompson, who is a dentist and clinical lecturer in primary dental care at the University of Manchester in the UK, the dental ...
LONDON, UK: Antimicrobial resistance (AMR) influences the success of medical treatment and allows for unhindered diffusion of bacteria. Although antibiotic ...
Live webinar
Wednesday, 3. June 2026
19:00 CET (Oslo)
Live webinar
Thursday, 4. June 2026
20:00 CET (Oslo)
Live webinar
Monday, 8. June 2026
18:00 CET (Oslo)
Live webinar
Monday, 8. June 2026
19:00 CET (Oslo)
Dr. Anthony Mak B.D.S, Prof. Marleen Peumans
Live webinar
Monday, 8. June 2026
20:00 CET (Oslo)
Live webinar
Wednesday, 10. June 2026
17:00 CET (Oslo)
Live webinar
Wednesday, 10. June 2026
20:00 CET (Oslo)
Nacho Fernández-Baca DDS, MSc



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East




























To post a reply please login or register