What do dentists want to know about occlusion? Occlusion may appear complicated because of the multiple factors involved, such as teeth, muscles and the temporomandibular joints (TMJs). It can also be confusing, owing to imprecise terminology and philosophies of occlusion.[1]
Philosophical disagreements have led to most of the confusion and resulted in several controversies. There is no consensus in the areas of diagnostic and treatment goals for occlusion.[2–4] This relates to a lack of agreement about the most physiological or functional mandibular position.[5, 6] Subsequently, the methods used to find such a mandibular position vary greatly. The techniques for interocclusal recordings are not standardised[7] and they include the use of wax, polyvinylsiloxane and computerised recordings.[8, 9]
Practising dentists are focused on how to plan a treatment and treat a patient, and occlusion is regarded as only a means to an end. Most dentists want to use simple, well-established and commonly accepted best clinical practices. Most dentists want to know how to record the bite for the laboratory.
Therefore, the purpose of this article is to clarify dental occlusion for practical clinical applications. First, the authors will propose a practical approach to occlusion based on three concepts: intercuspation, mandibular position and occlusal stability. Second, the authors will present a clinical decision guideline for occlusal recordings to use in daily practice. Third, the authors will present and compare the analogue and digital methods of occlusal recordings, placing emphasis on how to find and record centric relation.
A practical approach to occlusion
The concepts of intercuspation and mandibular position
All occlusal recordings are done at the tooth level. It appears that the recorded relationship is between the maxillary and mandibular teeth. Because the maxillary arch is fixed, the only variable is the position of the mandibular teeth. In a further analysis, the only variable is the position of the mandible. Therefore, occlusal recordings are inter-arch relationships at the tooth level.
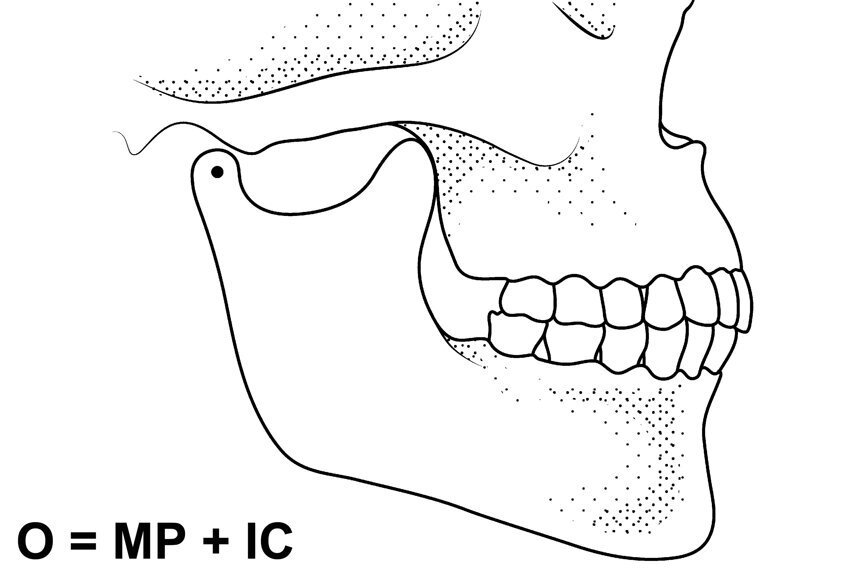
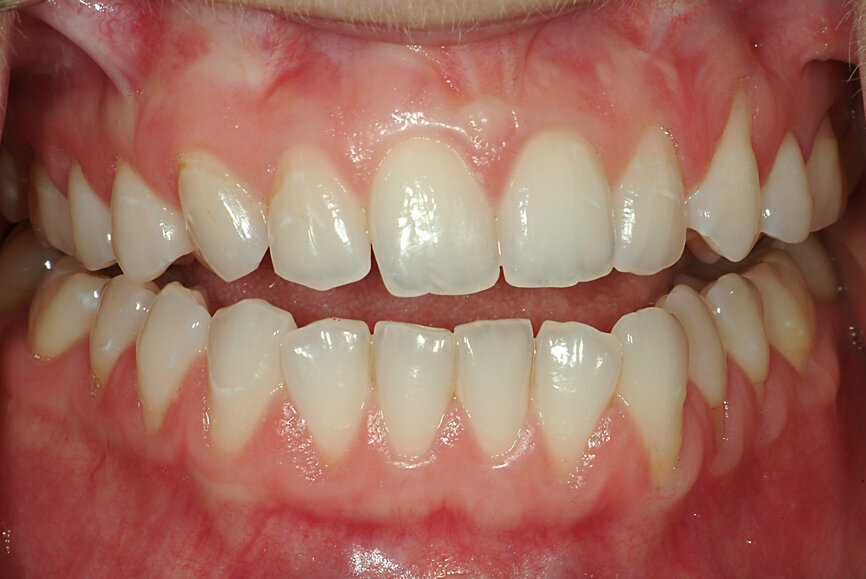
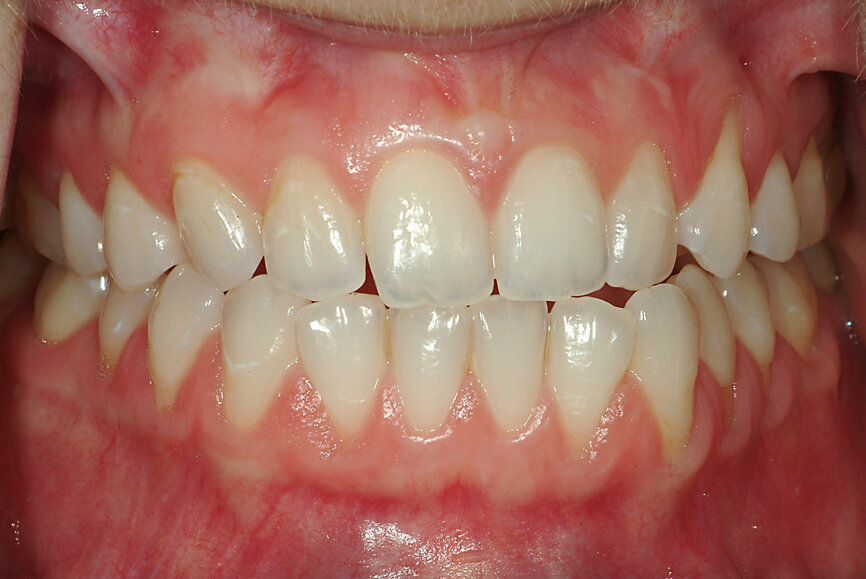
“Occlusion” is defined in the ninth edition of the Glossary of Prosthodontic Terms (GPT-9) as: “the act or process of closure” and “the static relationship between the incising or masticating surfaces of the maxillary or mandibular teeth or tooth analogues”.[10] Since the process of closure is of the mandibular teeth on to the maxillary ones, applying deductive reasoning, one can surmise that occlusion has two components mandibular position (MP) and intercuspation (IC). Any IC is always associated with an MP (Figs. 1 & 2). Occlusion is an MP when the teeth inter-cuspate.
We can express it with a mathematical formula: occlusion = MP + IC.
The concept of stability of occlusion
Like any natural system, occlusion seeks stability, which is accomplished through stability of the mandible. This may be obtained through a stable IC, sometimes named inter-cuspal position or maximal inter-cuspal position, and/or musculoskeletal stable joints (condylar position on the eminence).[11, 12] The GPT-9 describes “occlusal stability” as “the equalisation of contacts that prevents tooth movement”.[10] The authors refer here to the broader concept of the stability of occlusion as a total system.
McNeill describes three stable reference positions that may be used: inter-cuspal position, myocentric relation and centric relation.[13] In many clinical situations, the existing IC is widely accepted as a stable MP. Another stable reference position is centric relation (CR), which is a condylar-determined MP. CR is a stable musculoskeletal position of the condyles on the articular eminence or a condylar position. To be maintained, it has to be in harmony with a stable IC.[29]
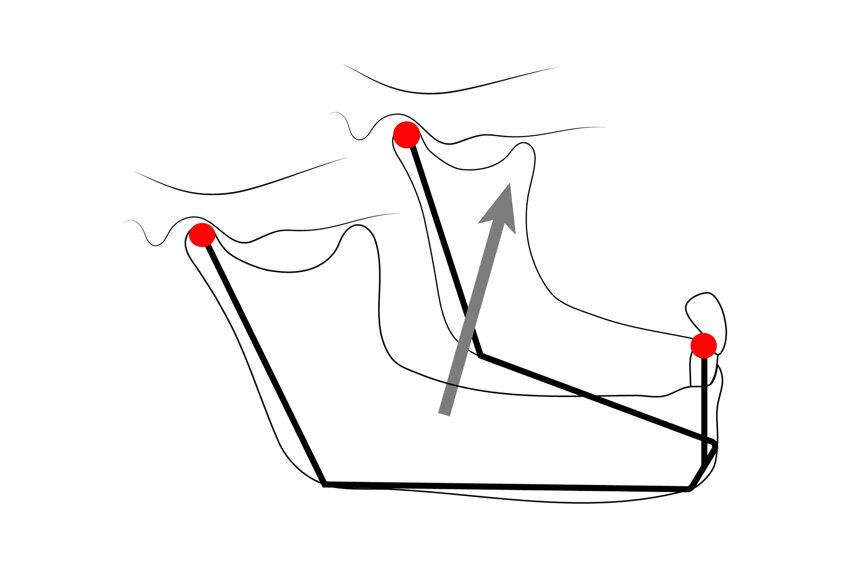
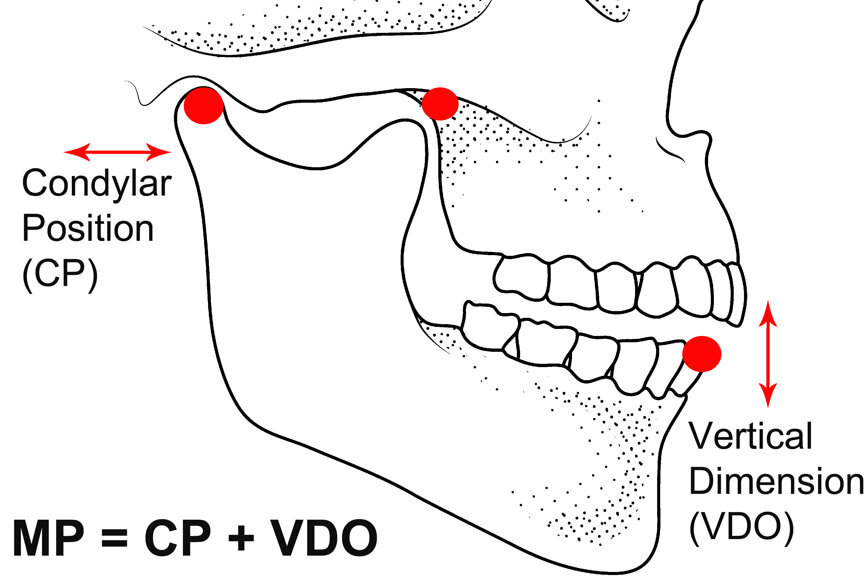
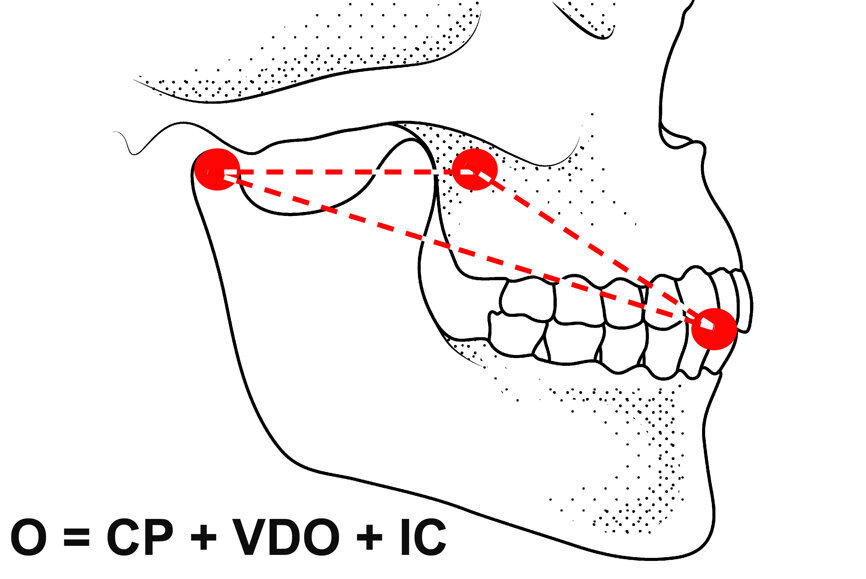
Let us analyse the MP concept further. Three non-collinear points, that is, that are not on the same straight line, can define the position in space of any solid object (Fig. 3). For increased precision, it is advantageous to select points as far apart as possible. The two condyles (first and second points) and the incisal point (third point) can define the position in space of the mandible relative to the anatomical structure of the maxilla/articular eminences (Fig. 4). The position of the condyles on the articular eminences can be defined as condylar position (CP). One stable CP, which is widely accepted, is CR. The position of the mandibular incisal point relative to the maxilla can be defined as the vertical dimension of occlusion (VDO). Using a mathematical formula: MP = CP + VDO. Therefore, the occlusion formula becomes (Fig. 5): occlusion = CP + VDO + IC.
Fig. 1: Mandibular position with condyles seated in the fossae and no intercuspation.
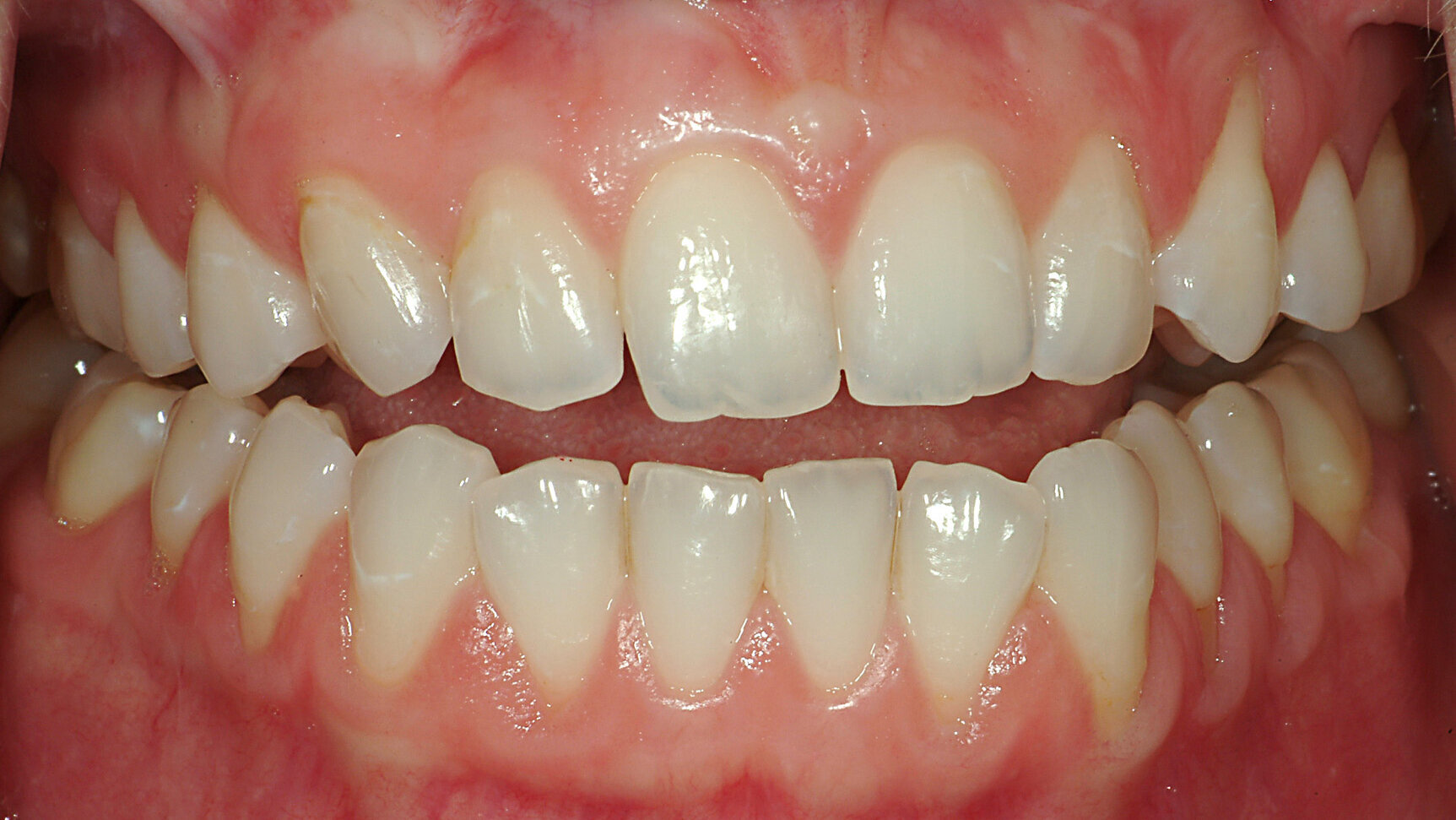
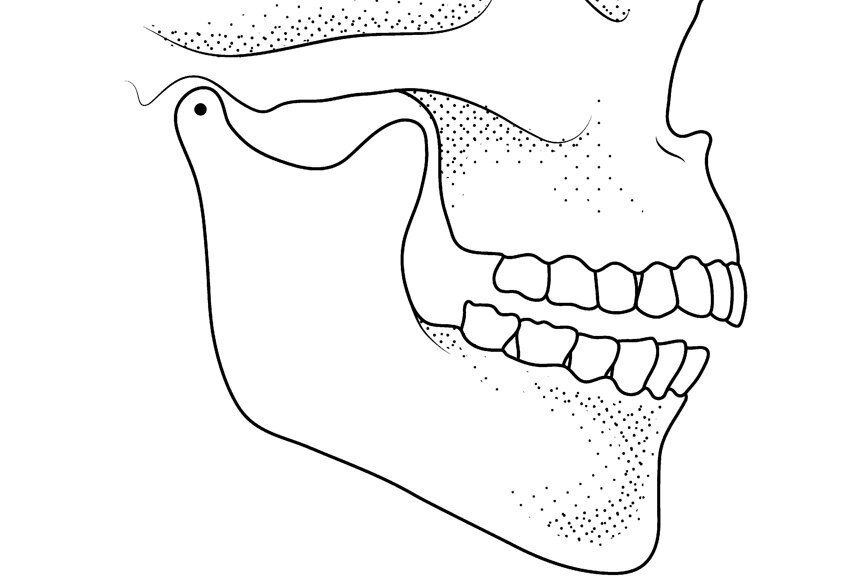
Fig. 2: Mandibular position with condyles down the eminence and maximal intercuspation.
Fig. 3: A drawing of the mandible, anterior teeth and fossae, showing a reversed tripod.
Fig. 4: Mandibular position defined as condylar position and vertical dimension of occlusion.
Fig. 5: Occlusion represented as mandibular position and intercuspation.
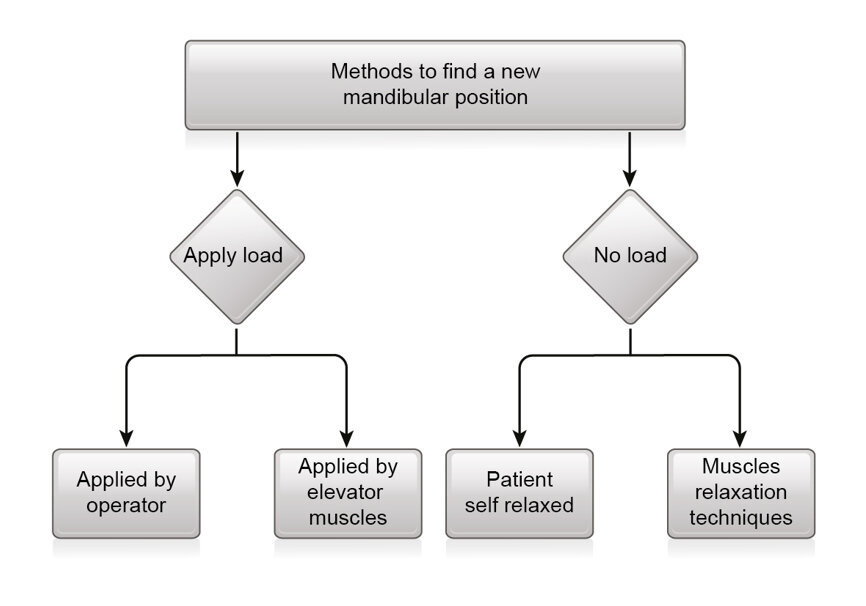
Fig. 6: Methods to find a new mandibular position.
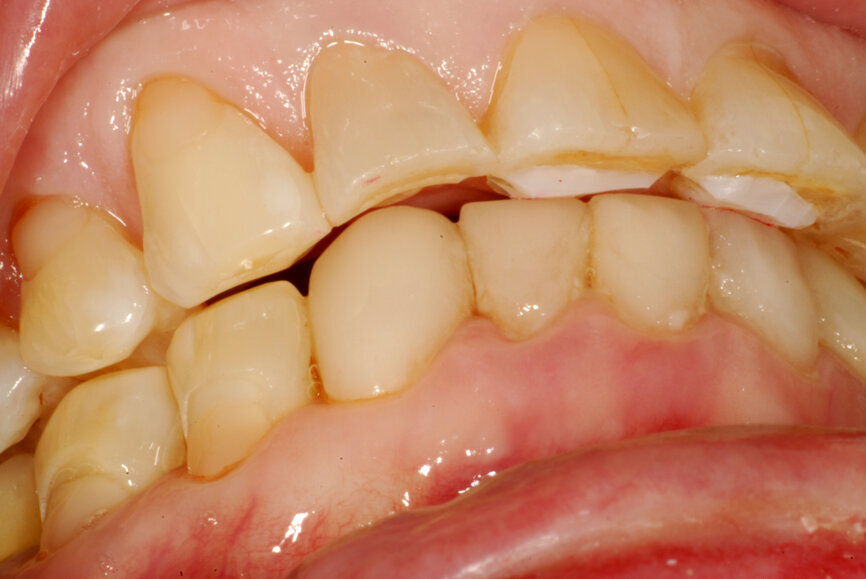
Fig. 7: Composite resin device creating a disclusion of posterior teeth.
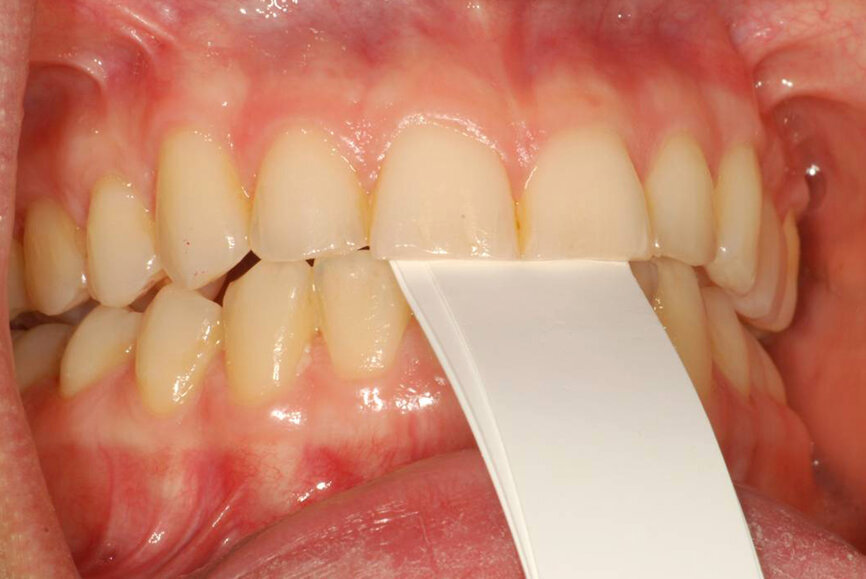
Fig. 8: Leaf gauge creating a disclusion of posterior teeth.
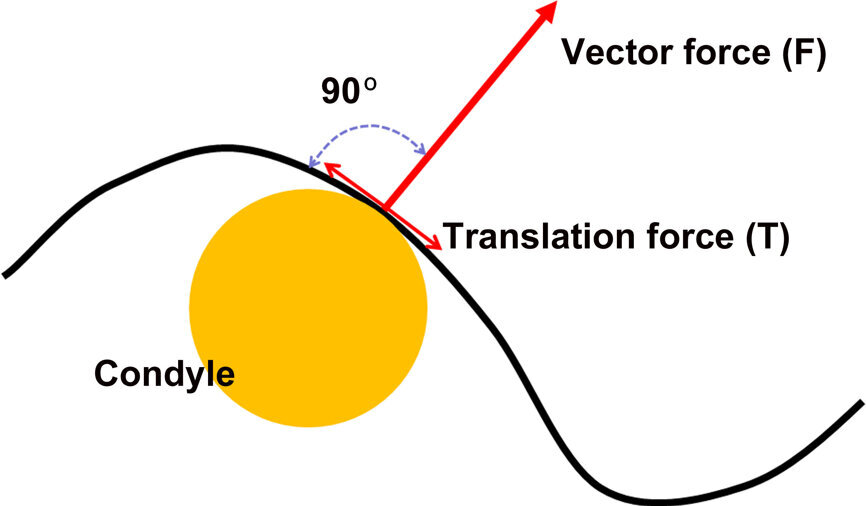
Fig. 9: The condyle position is based on the vector of force of the elevator muscles—perpendicular to the contour of the eminence.
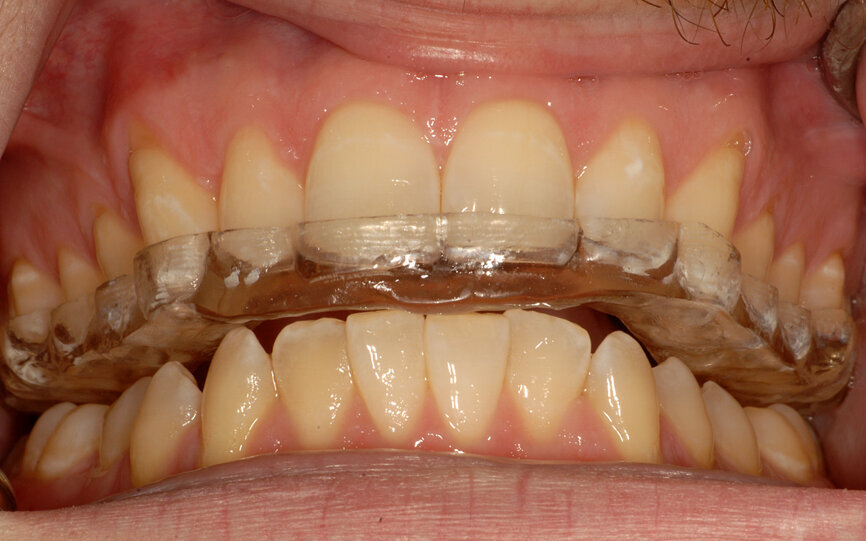
Fig. 10: A complete-coverage occlusal device to relax the muscles and heal the joints.
Fig. 11: Clinical decision guideline for occlusal evaluation and treatment.
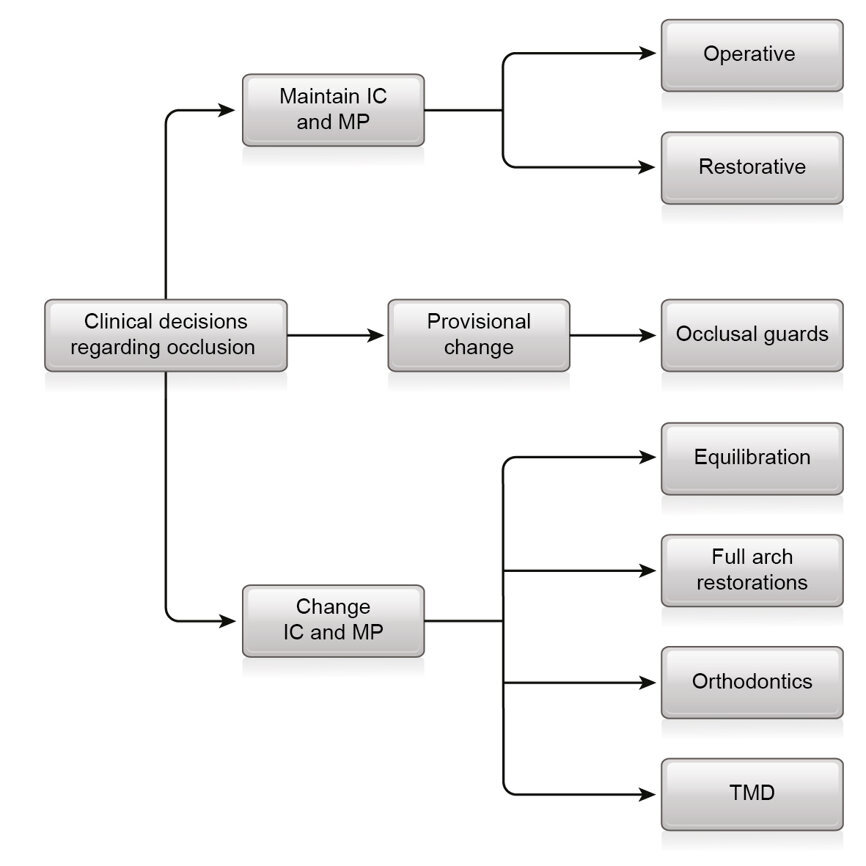
Fig. 12: Clinical decisions regarding occlusion. IC = intercuspation; MP = mandibular position; TMD = temporomandibular joint dysfunction syndrome.
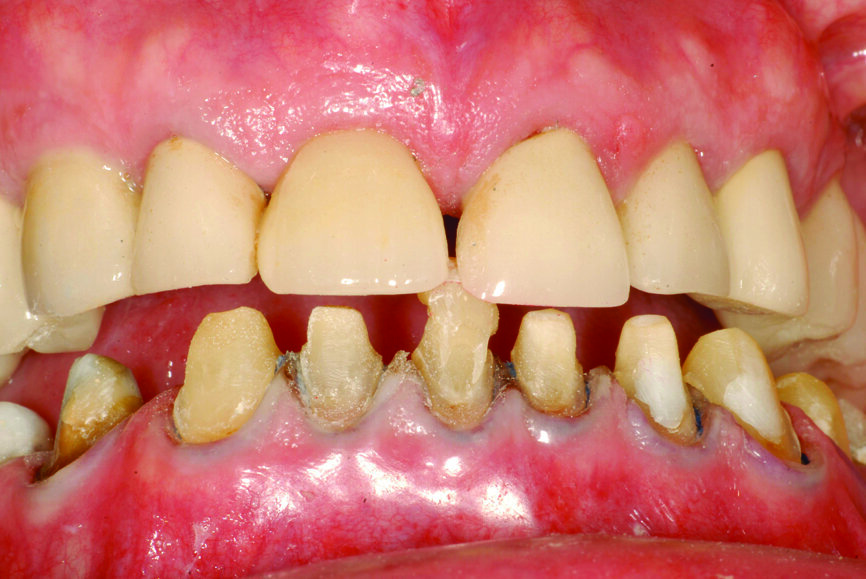
Fig. 13: Intercuspation requiring opening of the vertical dimension for restorative space.
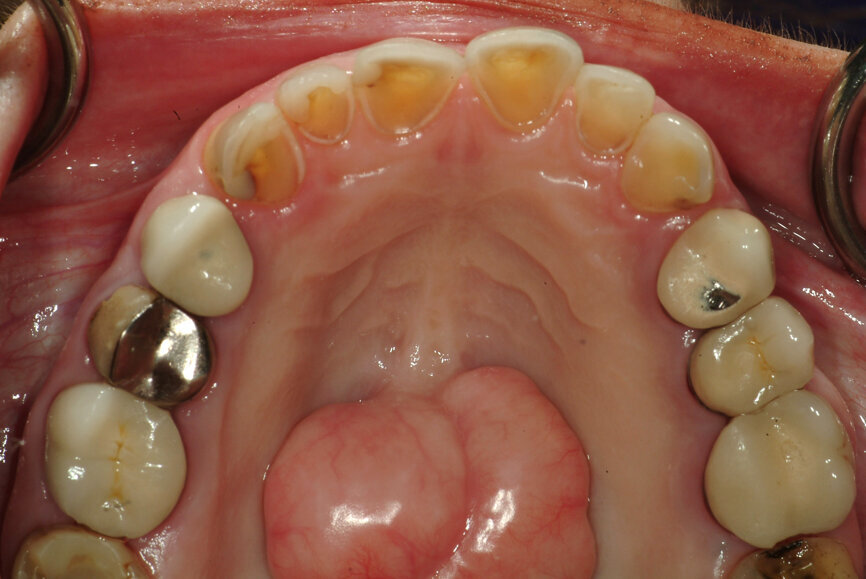
Fig. 14: Significant wear requiring occlusal coverage and altering
of occlusion.
Fig. 15: Occlusion with the mandible in centric relation and a significant open bite.
Fig. 16: Occlusion with intercuspation but a non-functional
mandibular position.
Fig. 17: Treatment modalities to recreate intercuspation in the new mandibular position.
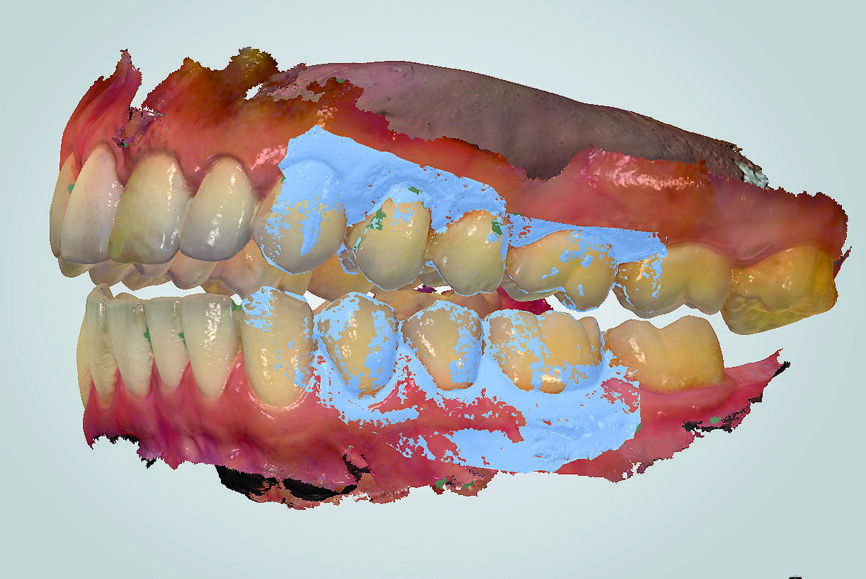
Fig. 18: TRIOS 3 software (3Shape) matching digital casts of arches to side view inter-arch scan (in light blue).
Fig. 19: Occlusal record limited to the prepared tooth area (when existing intercuspation is not altered).
Fig. 20a: Digital recording of intercuspation.
Fig. 20b: Digital recording of intercuspation.
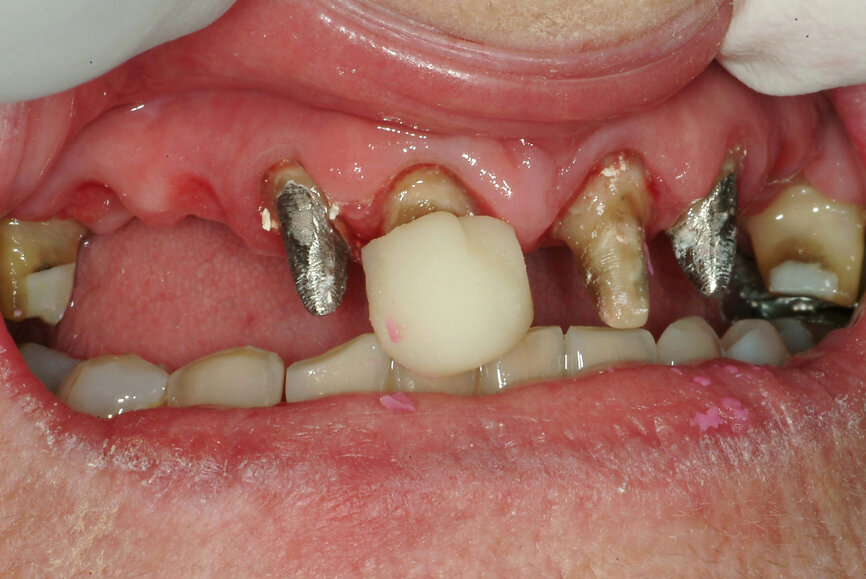
Fig. 21: Composite resin device at the desired vertical dimension of occlusion stabilises the mandible in centric relation.
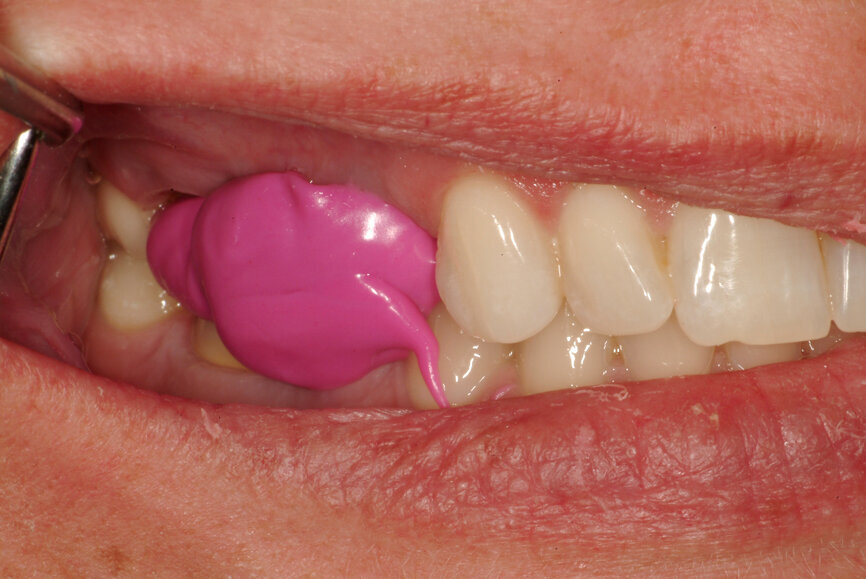
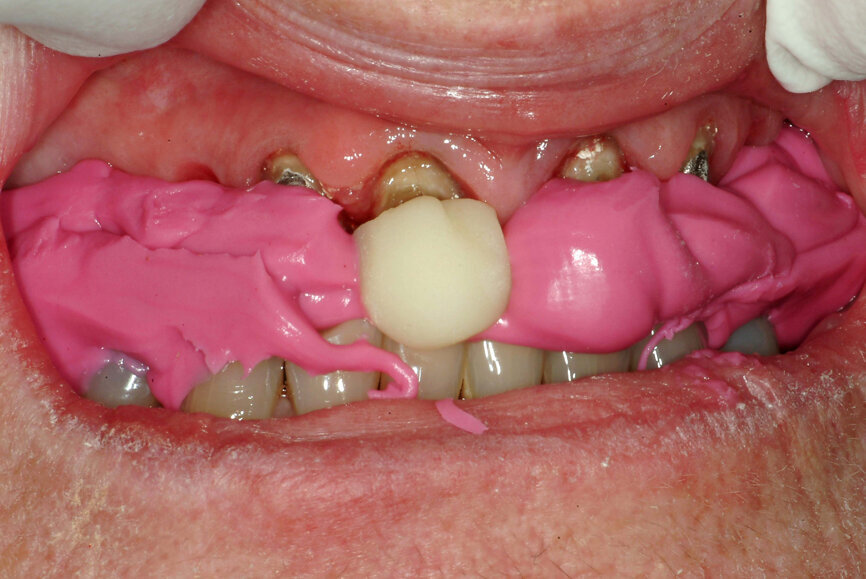
Fig. 22: Analogue recording of centric relation using a composite device to stabilise the mandible and polyvinylsiloxane recording paste.
Fig. 23: Analogue recording of centric relation using a composite device to stabilise the mandible and polyvinylsiloxane recording paste.
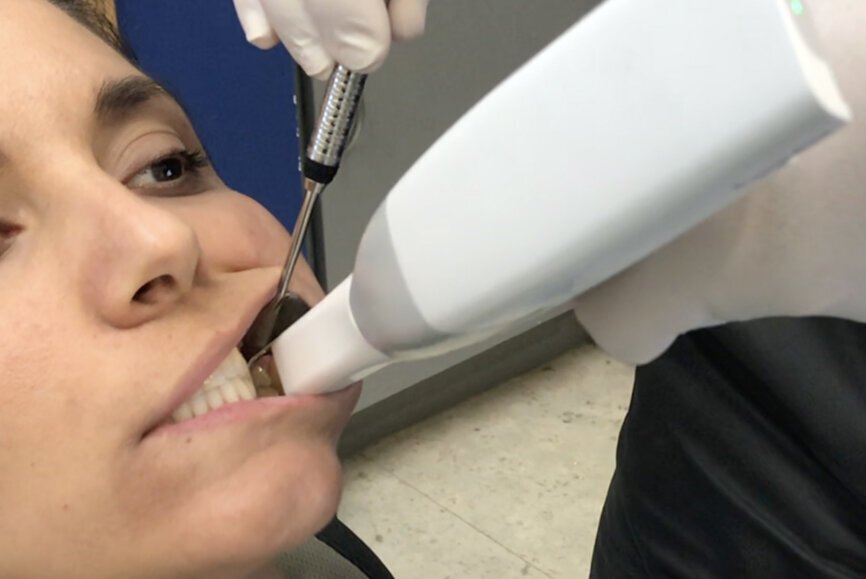
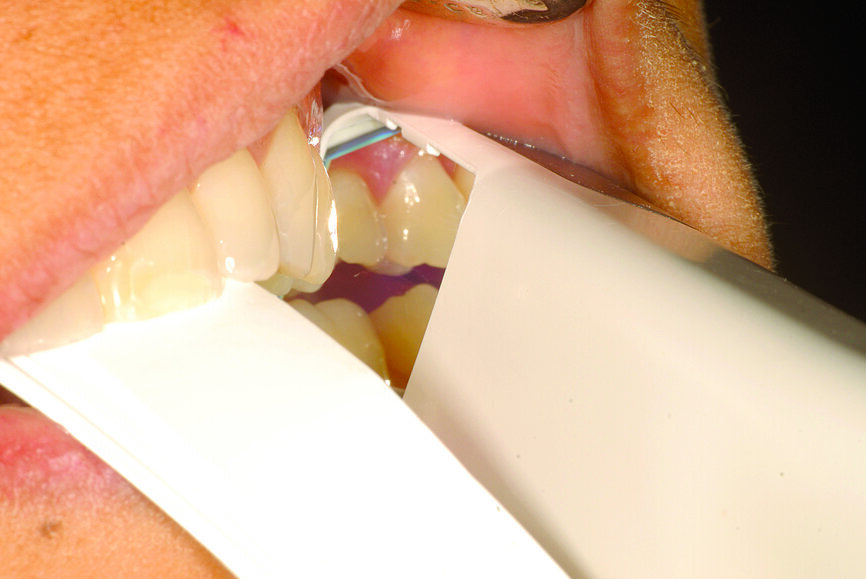
Fig. 24: Centric relation recording using an intra-oral scanner while the mandible is stabilised by a leaf gauge at the desired vertical dimension of occlusion.
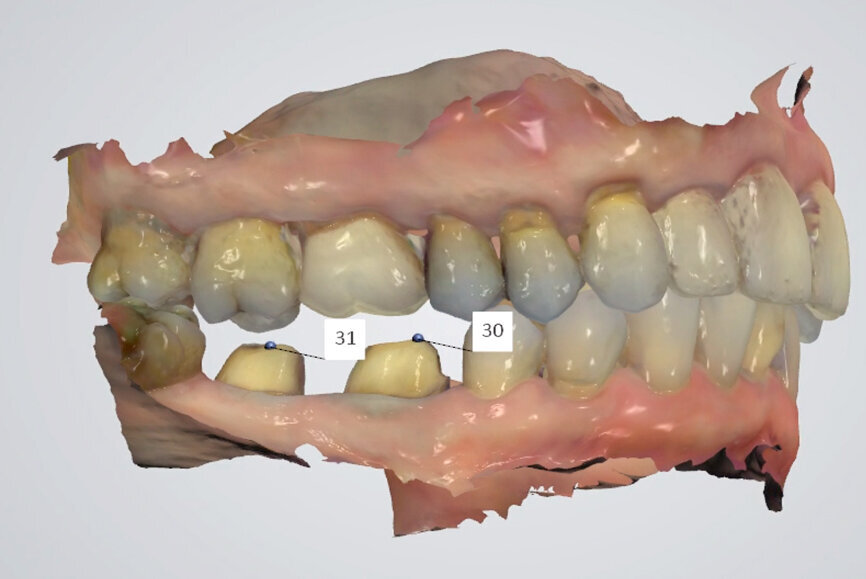
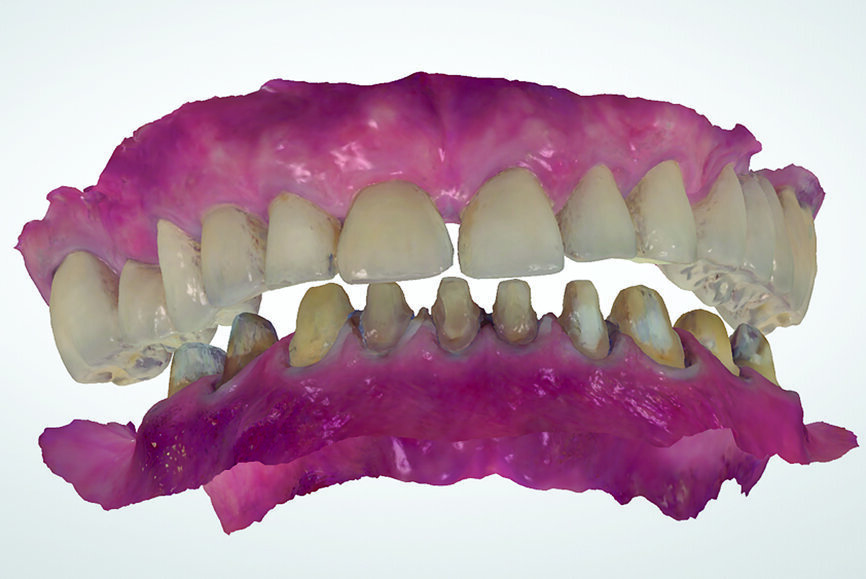
Fig. 25: Digital centric relation recording at the desired vertical
dimension of occlusion of all existing mandibular teeth, in preparation for a fixed complete denture.
Fig. 26: Digital recording of centric relation using a conventional finding method with a composite device at the desired vertical dimension of occlusion.
Fig. 27: Digital recording of centric relation using a conventional finding method with a composite device at the desired vertical dimension of occlusion.
These are the three variables we need to operate with, and these simplify occlusion by making it practical. Here are the clinical situations to which we can apply these simple occlusal rules.
When we decide to work with what is there, we accept the existing occlusion as functional; we accept the existing IC, but also the VDO and the CP as functional and acceptable for clinical use. When the MP is acceptable, it is irrelevant for that case; it can be considered to be zero, so the formula becomes: if MP = 0, then occlusion = IC.
When we decide to change the existing occlusion, or we do not have one at all (as in edentulous situations), we have to take all three variables into account. In general, all occlusal philosophies agree that VDO can be increased within the rotational movement of the condyles for aesthetic, functional and restorative purposes. The main differences in occlusal philosophies are related to the CP. The question becomes: what is an acceptable, physiological and long-term functional CP on the eminence? In other words: in what CP and VDO shall we create the new IC?
The case for a stable condylar position (centric relation)
In a stable occlusion, the IC guides the mandible in the same position repeatedly through muscle memory. When the IC is absent, the muscles may position the mandible in an endless number of positions, making reproducibility and stability a concern. Asking the patient to close in a “comfortable” position is an unpredictable means of finding a new MP.[14]
When the IC is absent, or the dentist decides to change it, the stability of the mandible has to be established with the help of the condyles and the VDO. The authors will make the case that the desired CP should be CR.
To determine a stable CP, we have two main options: to load or not to load the joints. It may appear that non-loaded, relaxed muscles is preferable. We want the patient to feel good and be relaxed, rather than forced into a particular position. However, there are inherent problems with relaxed, non-loaded positions:
- Relaxed positions can be in a large variety of CPs.
- Relaxed positions are very tricky to record—when we interpose a recording medium, the position may change.
- Most importantly, function and parafunction happen with contracted muscles and not in a relaxed position.
In healthy joints, loading creates a physiological, orthopaedically correct, predictable and reproducible CP.[11] Loading is actually a test of the health of the joints. There are two main ways to apply loading to the condyles: the bimanual manipulation technique[5] and the anterior obstacle technique.[14–16] The obstacle can be a leaf gauge, an anterior deprogramming device or a composite resin device. The anterior obstacle technique relaxes the lateral pterygoid muscles and positions the condyles in CR by contracting the elevator muscles (Fig. 6). These techniques are well documented and relatively easy to use.[18, 19]
When we accept CR as the stable CP, the MP formula becomes: MP = CR + VDO. Therefore, the occlusion formula becomes: occlusion = CR + VDO + IC.
When coupled with an anterior permissive obstacle of an adjustable size, such as a leaf gauge or a composite resin device, the mandible can simultaneously be placed at the desired VDO too (Figs. 7 & 8).
The bimanual manipulation technique is difficult to master and the mandible is difficult to stabilise, needing an interposed medium. The anterior obstacle technique is easier and allows the patient to find the individual CP on the eminences, based on the direction of the vector of force of the elevator muscles (Fig. 9).[20]
When patients exhibit tension, tenderness or pain upon loading the joints, a complete TMJ examination, both clinical and paraclinical (radiographs and MRI), needs to be done and a diagnosis needs to be established. The consensus of the literature is that a change in occlusion shall be done only after the joint and muscle issues have been resolved. In most cases, periodically adjusted occlusal device therapy of six to 12 weeks is recommended (Fig. 10). The authors do not address in this article the full extent of temporomandibular joint dysfunction syndrome issues, but recommend only proceeding with treatment after complete resolution of the problems.
The decision guideline for occlusal recordings to use in daily practice
Dentists have to decide how to treat the patient from an occlusal perspective. A guideline is needed because it simplifies and quantifies the decision process. The authors would like to enable every clinician to quickly evaluate, plan treatment for and treat any clinical situation from an occlusal perspective. What follows is a guideline for clinical decisions regarding occlusion (Fig. 11).
A guideline for clinical occlusal decisions
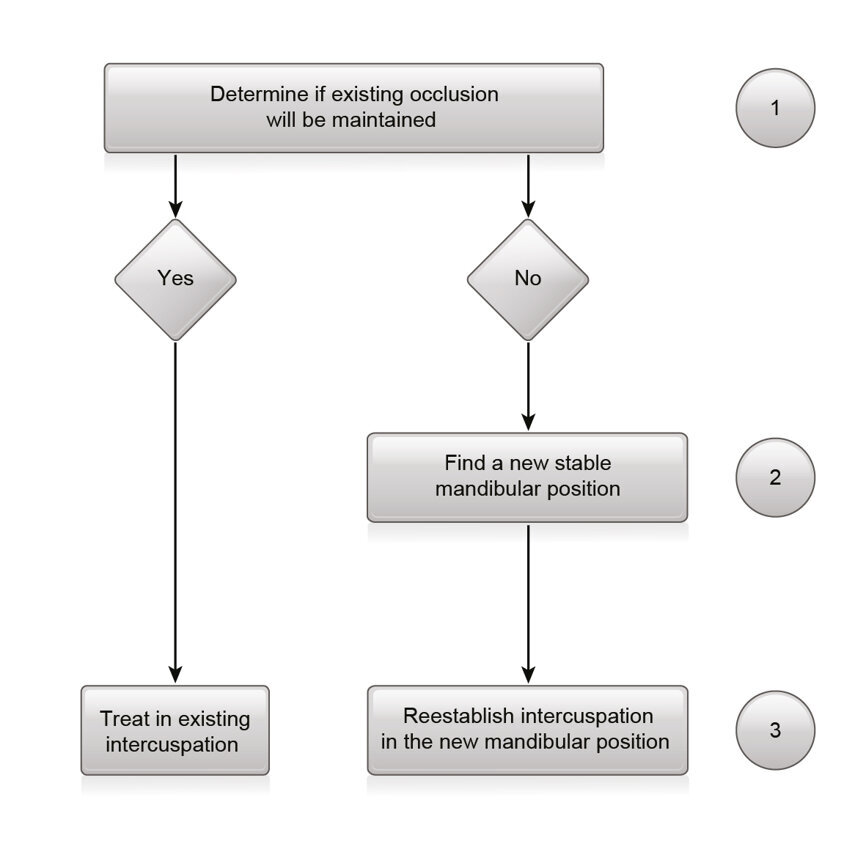
Step 1: Determine whether the patient’s present occlusion will be maintained
After a complete examination and diagnosis, the clinician designs a treatment plan regarding the three categories of problems: structure, function and aesthetics. Occlusion may be involved in all three aspects. The dentist needs to decide whether the treatment goals in each category can be achieved in the present occlusion (Fig. 12).
In the majority of clinical situations, the treatment can be done in the present occlusion. Fillings and single-unit or even multiple-unit fixed prostheses may be completed in the existing occlusion. The authors do not approve or disapprove of this process in the current paper, but only point out that, in their estimation, about 90 % of dental work is performed in the existing occlusion.
In summary, the first step is to decide whether the present occlusion will be maintained. If the present IC will allow the treatment to meet the patient’s objectives, proceed with treatment in that MP. If needed, record the existing IC and send the records to the laboratory. If a change in occlusion is needed, proceed to Step 2.
Step 2: Find a new stable and reproducible mandibular position, such as centric relation
To achieve the treatment goals, in some situations, the present occlusion has to be altered. The reasons may be structural, functional or aesthetic. The following is a simplified list of such instances:
- To obtain restorative space when needed restorations require an opening of the vertical dimension (Fig. 13);[21, 22]
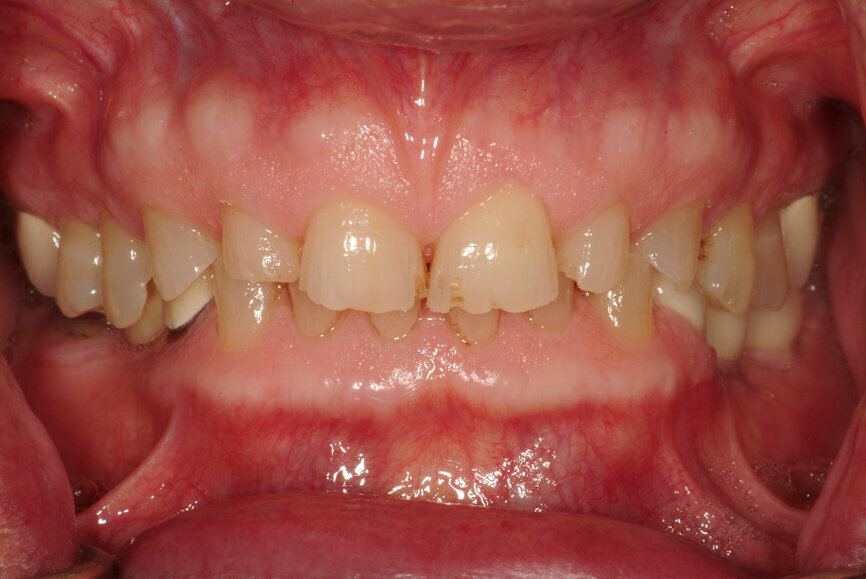
- when the occlusal signs are significant and the patient is made aware and accepts change to the occlusal relationship (Fig. 14);
- when the present MP creates functional problems (muscle and joint issues; Figs. 15 & 16). The simplest way to establish whether the MP is functional, even if the patient does not report symptoms, is the loading test.[23] When the loading test is positive, a change of MP, and subsequently of IC, may be needed.
As we have discussed, the desired MP to acquire is CR at the desired VDO. If needed, record the CR and send the records to the laboratory. Step 2 is always followed by Step 3.
Step 3: Re-establish intercuspation while preserving the new stable mandibular position (centric relation)
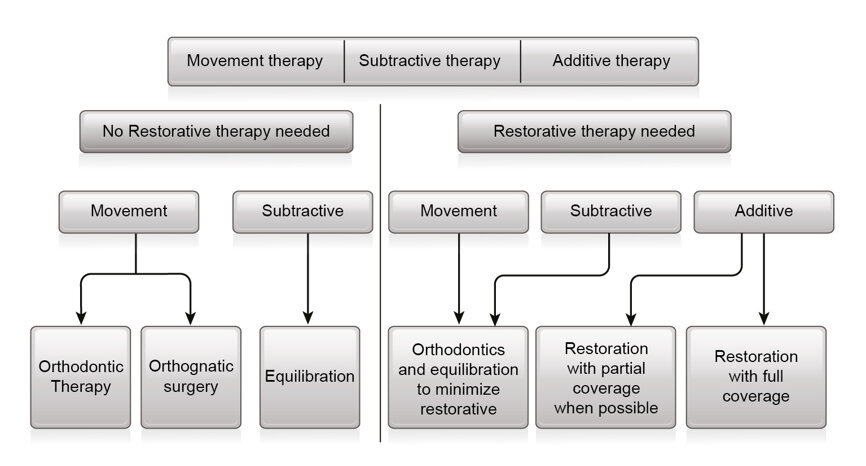
This newly acquired MP will have limited interdental contacts or no IC. An IC in harmony with the stable MP, that is, a stable CP, is needed for a functional occlusion. Therapeutic modalities to re-establish or reorganise inter-arch relations or IC are equilibration, movement of teeth or bone support, and restorative procedures. These modalities may be used alone or combined. The goal should always be to use the least invasive treatment while achieving the patient’s objectives (Fig. 17).
In summary, the third step is to ensure that the new occlusion is stable and functional. Re-establish IC by using the least invasive treatment that allows achievement of the patient’s objectives.
Analogue and digital occlusal recordings of existing intercuspation and centric relation: Clinical protocols
Historically, occlusal recordings were performed using wax wafers, wax rims on base plates and bite registration pastes, such as polyvinylsiloxane. With the introduction of contactless 3D impressions using intra-oral scanners, new techniques for occlusal recording have emerged.
The classic analogue technique requires a recording medium (waxes, polyvinylsiloxane) to be interposed between the arches. The interposition of any material in between the teeth or arches is an obstacle that the patient may avoid or try to accommodate for, thereby skewing the recording. The record itself may distort during transportation to the laboratory. The laboratory step of fitting the occlusal record on to the stone casts and mounting the assembly in the articulator is also prone to significant errors.
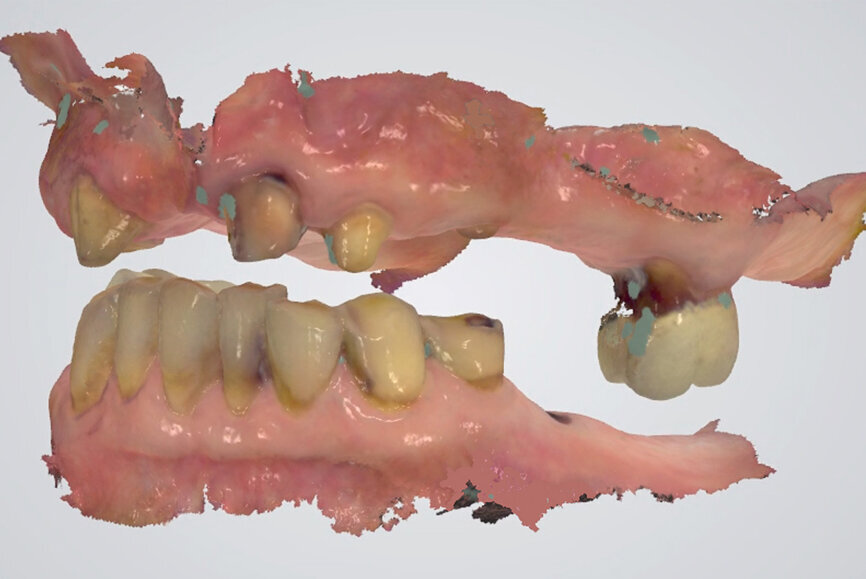
In contrast, digital recording has several advantages regarding efficiency and accuracy. The recording takes place without an interposed medium. The uploading of the digital casts in the software to the IC or CR position happens without the need for positioning of physical stone casts by an operator (technician). This ensures an accurate and efficient mounting in the virtual articulator. The direct digital occlusal recording is based on the intra-oral scanner software matching the digital casts of the arches to the inter-arch scan obtained from the side view of the arches (Fig. 18). The only noted disadvantage of the direct digital recording relates to the additional cost of acquiring an intra-oral scanner and the learning curve associated with operating one.
Occlusal recordings of existing intercuspation
When the dentist decides to maintain the existing bite, that is, to work with what is there, the focus should be on ensuring that there is no unwanted change in the recording and transmission to the laboratory. Analogue recordings of existing IC can be performed using polyvinylsiloxane registration pastes or waxes (Fig. 19). Dental laboratories usually digitise the analogue records and fabricate the restorations digitally. The process of digitisation can introduce imprecisions, owing to the difficulty of the laboratory articulating the models in the precise position. Digital recordings of existing IC can be performed using intra-oral scanners. The scanner is placed in the buccal corridor and records the relative position of the maxillary and mandibular teeth (Figs. 20a & b).
Occlusal recordings of non-existent intercuspation/centric relation
The technique for finding and recording CR described in this section can be used in different clinical situations, such as one full arch of fixed partial dentures, or for occlusal devices. It also incorporates the recording at the desired VDO. The process of finding CR is done conventionally using an anterior device, such as a leaf gauge or a composite resin device. There are devices that attempt to find the CR digitally, but these are not the subject of this paper.
The described technique uses an anterior obstacle. The anterior obstacle is a valuable tool that stabilises the mandible, allows the clinician to choose the desired VDO and facilitates the inter-arch recording with analogue or digital methods. The anterior obstacle technique appears simpler and less prone to errors than similar techniques are because the mandible is more stable when supported by an anterior obstacle.
The recommended technique for finding the CR position in a clinical situation with all teeth in one arch prepared for restorations:
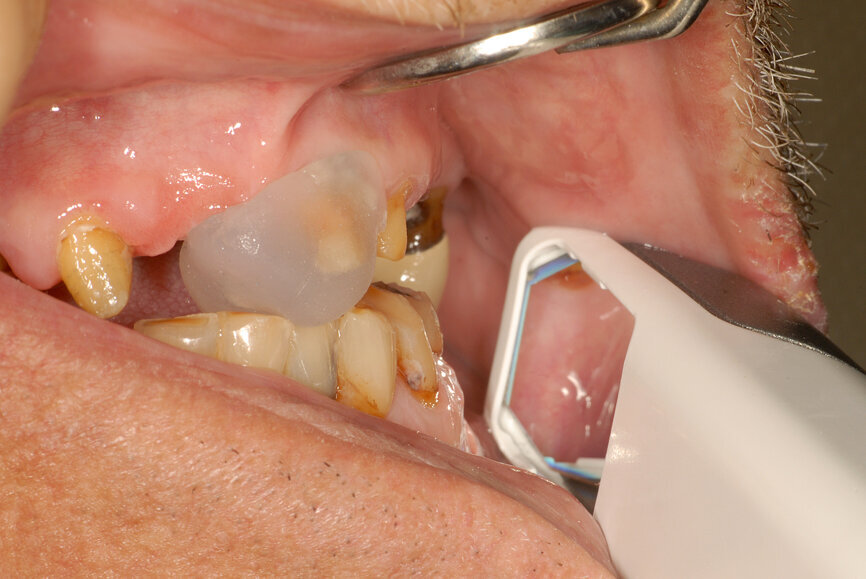
- Create a composite resin device (stop) on an anterior tooth (Fig. 21) at an approximate VDO to allow restorative space.
- Ask the patient to move the mandible forward and backwards two to three times. That will relax the lateral pterygoid muscles and allow the elevator muscles to position the condyles in a physiological position on the eminences.
- Adjust the composite resin device, using articulating paper, for a smooth mandibular movement. Also, adjust the height until the desired VDO is reached—evaluate the anterior space first, then the posterior space and then adjust the prepared teeth if needed to gain the appropriate restorative space.
- After the adjustments, ask the patient to maintain the backward position. That can be considered CR.
The technique for recording the CR position can be performed using analogue (Figs. 22 & 23) or digital methods (Figs. 24–27).
Conclusion
Occlusion can be seen as a combination of IC and MP. Most of the time, dentists can restore in the existing IC. In those cases, the process is straightforward: the occlusal record is of the given bite (existing occlusion). When the IC is absent or has to be altered, the dentist should position the condyles in an orthopaedically stable position (CR). The authors recommend finding the CR using an anterior obstacle and loading of the elevator muscles. At the same time, the desired VDO can be established. Subsequently, one may record that position with analogue or direct digital methods. In the authors’ opinion, digital methods have several advantages, including their accuracy, ease of technique and ease of evaluation, and the capability of mounting in a virtual articulator without any other intervention.
Editorial note: A list of references is available from the Publisher. This article was published in CAD/CAM―international magazine of digital dentistry Vol. 10, Issue 3/2019.



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East



























To post a reply please login or register